Neurodiversity Celebration Week (16–20 March 2026)
Encourages organisations to recognise neurological difference as part of the natural human variation. That recognition matters. But recognition without reform risks becoming symbolic or performative.
In my coaching work with neurodivergent workers, I hear a consistent story. Highly capable people describe working twice as hard to meet performance expectations that were not designed with them in mind.
Many avoid diagnosis because of the expense or because if are diagnosed they may have a positive duty to disclose and in some occupations, a diagnosis of ADHD, especially where stimulant medication has been prescribed can spell the end of their career.
Others share a reluctance to disclose because they are uncertain how disclosure would change how they were perceived. Others reveal how they have been treated after disclosing their neurodivergence to their employer and asking for adjustments. Denied any consideration of adjustments and questioned as to the legitimacy of their “disability” and required to provide proof that they adjustments requested are required on genuine disability grounds.
Then they find themselves subjected to increased levels of supervision and performance monitoring that increased their feelings of vulnerability and created anxiety which led to a deterioration in their neurodivergent functioning and further deterioration in work performance.
Often my organisational clients often express a different but related challenge. Leaders want to be inclusive, yet they feel constrained by compliance frameworks. They may ask, “What’s the minimum we’re required to do?” rather than “How should we design work so that it is safe and inclusive for everyone?”. Or they recognise their neurodivergent worker’s exceptional talents but don’t understand why their performance is not consistent or why they communicate in atypical ways and feel they need to find ways to make the worker conform. Others refer workers to me for coaching because the worker is already on a performance improvement plan and then discloses that perhaps the reason for their difficulties is their neurodivergence.
The conversation becomes procedural rather than preventative.
If we are serious about improving outcomes for neurodivergent Australians, we must examine how our disability employment systems actually operate. The prevailing model (“diagnose, disclose, prove, then adjust”) was designed to protect workers with disabilities.
However, in practice when applied to neurodivergent workers, it often does the opposite.
This is not a marginal issue. Neurodivergence is common. International estimates suggest 15–20 per cent of the population is neurodivergent (Doyle & McDowall, 2021), and about 65% are of working age. A conservative estimate is that at least one in ten workers in any workplace has a neurotype such as ADHD, autism or dyslexia. In sectors like IT, construction and engineering, that proportion may be significantly higher.
Yet our policy frameworks are built as if neurodivergence is rare and exceptional.
That mismatch matters.
The Legal Framework – Protection Triggered by Proof
Under the Disability Discrimination Act 1992 (Cth) (DDA), ADHD, autism, dyslexia and other neurotypes fall within the statutory definition of disability. On paper, that provides protection. In reality, protection is activated only once a worker can demonstrate that they meet a legally recognised threshold.
As explored in ADHD/ADD, the Workplace and Discrimination (Arnold et. al., 2010), Australian discrimination law reflects a medically anchored model of impairment. The law asks whether an individual fits within a category. It does not begin by asking whether workplace systems themselves are producing disadvantage.
In most workplaces, this translates into a familiar sequence:
- Diagnosis;
- Disclosure;
- medical evidence; and then
- consideration of “reasonable adjustments”.
It appears orderly. It appears fair. But it rests on assumptions that frequently collapse in practice.
The Assumptions That Don’t Hold
-
The first assumption is that neurodivergent adults are diagnosed.
In most cases they are not. The 2023 Senate Inquiry into ADHD assessment and support services documented long waiting periods, significant out-of-pocket costs and shortages of trained clinicians, particularly in regional and First Nations communities (The Senate Community Affairs References Committee, 2023). Raman et al. (2018) estimate that only a minority (about 1:10) of Australian adults with ADHD are formally recognised and treated. The diagnostic gap reflects barriers to access, not absence of neurodivergence.
-
The second assumption is that diagnosis is accessible.
For many, it is financially prohibitive. Private assessments can cost thousands of dollars. Public pathways are limited. Culturally safe services remain uneven. When workplace protections hinge on medical certification that is practically unattainable, access to safe work becomes contingent on personal resources (The Senate Community Affairs References Committee, 2023).
-
The third assumption is that individuals identify as “disabled”.
Many neurodivergent adults do not conceptualise their neurotype as a disability. Some view it as a difference. Others have developed strategies that allow them to function, albeit with significant effort. Requiring someone to adopt a legal disability label before adjustments are considered introduces an additional psychological barrier. Legal categorisation is blunt; lived identity is nuanced.
-
The fourth assumption is that disclosure is safe.
For hidden disabilities, disclosure is a calculated risk. Workers may fear stigma, reduced career prospects or subtle exclusion. These concerns are not hypothetical. Litigation regularly turns on whether an employer knew about a disability and whether adverse treatment was because of it.
In Debus v Condor Energy Services Ltd [2022], the Court grappled with whether the employer had sufficient knowledge of the worker’s autism and whether that knowledge could be causally linked to the alleged adverse action. The dispute did not centre on whether autism exists, but on whether it had been clearly disclosed and understood.
Similarly, in Kristjansson v State of Queensland [2018], the Court accepted the existence of disability but rejected the discrimination claim after examining whether the requested adjustments were “reasonable” in the circumstances. Even where disability is acknowledged, the litigation frequently turns on proportionality, practicality and evidence.
When Legal Tests Obscure Real Risk
The case law reveals a recurring pattern. Arguments become absorbed in technical analysis. How much did the employer know? When did they know it? Was the adjustment formally requested? Would providing it impose unjustifiable hardship on the employer? Was the request proportionate?
Those questions are doctrinally sound. They reflect how discrimination law is structured.
However, they tend to work more cleanly in cases involving visible or widely understood disabilities, where the existence of impairment is not contested and where social stigma and misinformation are less pronounced. In those contexts, disclosure is clearer, knowledge is easier to establish, and adjustments are often more tangible.
Neurodivergence is different.
It is frequently invisible. Often undiagnosed and misunderstood. It carries persistent stereotypes about competence, reliability and behaviour. The very traits that require adjustment may also be misinterpreted as performance deficiency or attitudinal problem.
As a result, disputes involving neurodivergent workers become preoccupied with evidentiary thresholds such as whether there is medical proof of a diagnosis, whether the disclosure was formal and documented such that the employer could be in no doubt, and whether the requested adjustments were precise and proportionate.
In this way, the legal process as it is typically applied by employers can unintentionally increase risk. The worker must first prove disability. Then prove disclosure. Then prove that the requested adjustment is reasonable.
Meanwhile, the question of whether withholding the requested adjustment creates a foreseeable risk of harm to the worker rarely receives equivalent scrutiny.
Yet perhaps that is the more important question.

Instead of asking only whether providing an adjustment would impose unjustifiable hardship on the employer, we might also ask, would failing to provide the adjustment create unjustifiable hardship to the worker?
For neurodivergent workers, the answer can be profound. Unaddressed sensory stress, executive functioning strain, chronic anxiety associated with misaligned performance systems can escalate into burnout, psychological injury and ultimately the ending of the employment relationship, one way or the other. Then potentially financial stress, career and reputational harm. The harm is not theoretical. It is cumulative and measurable. Neurodivergent workers experience mental health injuries at more than twice the rate of neurotypical workers and higher unemployment, lower earning capacity and more job insecurity than their neurotypical peers.
When the legal inquiry focuses narrowly on employer burden, the analysis risks overlooking worker risk.
A system that weighs hardship on one side but fails to meaningfully assess harm on the other is structurally incomplete.
When Compliance Becomes a Trap
Paradoxically, the less safe disclosure feels to the worker, the less likely it becomes. The less disclosure occurs, the easier it is to frame workplace consequences as performance issues rather than manifestations of unmet support needs.
Anti-discrimination law is reactive. It responds after adverse treatment or hardship occurs. It is structured around individual complaints and proof.
This design can unintentionally create a disclosure trap. Workers who disclose face stigma or subtle judgement. Those who choose not to disclose risk having emerging difficulties managed as performance issues. When conflict arises, the focus often shifts to technical questions like whether the employer had sufficient knowledge of the disability and whether the disability was the cause of the performance concerns.
In this way, inclusion becomes conditional and contested rather than embedded. The system may technically comply with statutory obligations while still producing avoidable harm.
A Safety Lens Changes the Question
The limitations of this model become clearer when viewed through work health and safety principles.
Under section 19 of the Work Health and Safety Act 2011 (Cth), employers owe the primary, non-delegable duty to ensure, so far as reasonably practicable, the health and safety of workers. That obligation is proactive. It does not depend on diagnosis. It does not require medical evidence before hazards must be identified and controlled.
Foreseeable psychosocial risks such as sensory overload, unclear or confusing instructions and expectations, inconsistent supervision or rigid performance metrics exist and can impact all workers, whether or not someone has disclosed a neurodivergent condition. Waiting for proof of a disability before redesigning the work to eliminate these psychosocial risks is like waiting for a worker to fall and break a leg before implementing falls prevention controls.
Its inconsistent with contemporary risk management.
From a safety perspective, the relevant question shifts. It is no longer “Has this worker a proven disability?” It becomes “Does this system of work create a foreseeable risk of injury for a significant proportion of our workforce?”
Given prevalence rates, the answer is often yes.
The Economic Consequences of Delay
The cost of inaction is measurable.
Deloitte estimated that ADHD alone cost the Australian economy more than $20 billion in a single year, with productivity losses including absenteeism, presenteeism and reduced workforce participation forming the largest component. Employers bore the greatest share of those costs (Deloitte Access Economics, 2019).
The 2022 Senate Select Committee on Autism described life outcomes for autistic Australians as “unacceptably poor”, including markedly higher unemployment rates and reduced life expectancy (Select Committee on Autism, 2022).
These are not abstract statistics. They reflect cumulative systems failure across healthcare, education and employment.
When organisations defer inclusion until diagnosis is proven, they are not containing cost. They are deferring it into turnover, absenteeism, sick leave, burnout, workers’ compensation claims, litigation risk and lost innovation and productivity.
Moving Beyond the Medical Model
At the heart of the problem lies the stubborn persistence of the medical model of disability in employment. It locates the issue within the individual and treats adjustment as an exception to an otherwise neutral system.
But work systems are not neutral. They are typically designed around neurotypical norms including linear communication, sustained attention, rapid task switching, sensory tolerance, one-size-fits all approaches to recruitment, training and performance management.
Contemporary biopsychosocial approaches recognise that disability often emerges from the interaction between individual characteristics and environmental design. From this perspective, the question changes.
Instead of asking, “What is your diagnosed disability?” we ask, “How does our work design interact with different cognitive styles?”
Clear communication, flexible structures, predictable processes and supportive supervision benefit everyone. Universal design reduces reliance on disclosure, allows workers with differing abilities to work with in the system without having to disclose or ask for adjustments and strengthens psychological safety.
It shifts inclusion from reactive accommodation to intelligent and universal system design.
Designing for Reality, Not Exception
Neurodiversity is already present in every workplace whether it’s diagnosed or not and whether it’s disclosed or not.
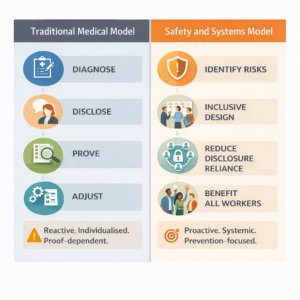
The traditional “diagnose–disclose–prove–adjust” model may satisfy minimal compliance requirements. But it remains reactive, individualised and dependent on vulnerable neurodivergent workers taking all the risk and providing proof that may not be accessible to them.
A more mature approach recognises scale. It integrates neuroinclusion into governance, recruitment, performance management and safety systems from the outset.
This is not about lowering standards. It is about designing work that reflects the cognitive diversity that already exists.
When I speak with neurodivergent professionals, what they want is not special treatment. They want clarity, predictability, fairness and the opportunity to use their strengths without being penalised for difference.
When I speak with organisations, what they want is practical guidance, not just legal compliance, but sustainable systems that reduce risk and improve performance. They are often surprised to discover that the same structural changes that support neurodivergent workers improve outcomes for everyone.
The gap between these two perspectives is rarely about intent. It is about design.
Neurodiversity is already present in every workplace whether it’s been diagnosed or not, and whether it is disclosed or not. The question is not whether the law can respond once disadvantage occurs. The question is whether we are prepared to design work in a way that prevents it.

